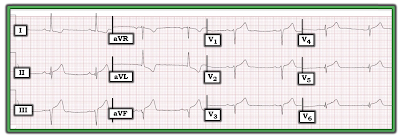
The patient is a man in his 70s — with symptoms for the past 3 days. He presented to the ED with worsening chest pain. His initial ECG is shown in Figure-1.
QUESTIONS:
- Should you activate the cath lab?
- How many of the 12 leads manifest abnormal ST-T wave changes?
- Is the low voltage a relevant finding?
 |
| Figure-1: Initial ECG in the ED — obtained from a man in his 70s with 3 days of chest pain. (To improve visualization — I've digitized the original ECG using PMcardio). |
=======================================
NOTE: Some readers may prefer at this point to listen to the 4:00-minute ECG Audio PEARL before reading My Thoughts regarding the ECG in Figure-1. Feel free at any time to refer to My Thoughts on these tracings (that appear below ECG MP-80).
=======================================
Today's ECG Media PEARL #80 (4:00 minutes Audio) — Reviews the ECG finding of Low Voltage (and potential clinical implications of low voltage in the setting of acute MI).
=============================
MY Approach to the ECG in Figure-1:
As always — I favor a Systematic Approach for interpretation of every ECG I encounter (This Systematic Approach is reviewed in ECG Blog 205).
- Rate & Rhythm: The rhythm is sinus at ~70/minute.
- Intervals: The PR, QRS and QTc intervals all appear normal.
- Axis: The frontal plane QRS axis is normal (close to zero degrees — as the QRS complex in lead aVF is nearly isoelectric).
- Chamber Enlargement: None
PEARL #1: Did YOU note the relatively Low Voltage throughout this tracing? Although strict criteria for low voltage are not quite met in this tracing (ie, the QRS complex in all 6 limb leads is not ≤5 mm — because the R wave in lead I is taller than this). That said — 5 of the 6 limb leads satisfy this low voltage criterion — and all 6 chest leads are of small amplitude!
- As we are about to contemplate the possibility of acute or recent infarction — it is helpful to be aware of potential causes associated with low voltage.
- Relevant potential causes of Low Voltage to consider in today's case include: i) Pericardial effusion; ii) Takotsubo cardiomyopathy; and, iii) A large acute (or recent) infarction, that may result in myocardial "stunning" (See the above Audio Pearl and/or ECG Blog #262 for more on this subject).
Continuing My System — Regarding Q-R-S-T Changes:
- Q Waves — Assessment is challenging because of the small amplitude of the beats in lead III, and especially in lead aVF. That said — a QS wave is seen in at least 2 of the 3 beats in lead III. It looks like an ever-so-tiny initial positive deflection (r wave) is present in the middle beat in this lead.
- I find it even more difficult to assess lead aVF for the presence of Q waves — as QRS amplitude is tiny (no more than 2 mm) in this lead. What can be said about lead aVF — is that all 3 of the beats that we see in this lead are notched (ie, fragmented).
PEARL #2: The finding of an isolated QS complex in lead III and/or lead aVF is not diagnostic of previous inferior infarction.
- Higher specificity for the occurrence of inferior infarction at some point in time is only obtained when Q waves of a "certain size" (ie, larger and/or wider than normal septal q waves) are seen in all 3 inferior leads (ie, leads III, aVF and also lead II).
- That said, in my experience — the finding of an isoelectric or predominantly negative QRS complex that is fragmented in one or more inferior leads (as seen in lead aVF in Figure-1) — significantly increases the likelihood that inferior infarction occurred at some point in time.
- In Figure-1 — there is no Q wave in lead II. As a result — the question of a QS complex in lead III by itself does not reliably predict inferior infarction at some point in time. However, in association with the tiny, notched (fragmented) complex in lead aVF — I'd suspect an inferior infarction may have occurred at some point. Whether this event began 3 days ago (at the time of symptom onset in today's patient) — or whether the inferior infarction is old and unrelated to the ST-T wave changes we are about to assess in the chest leads — can not be determined from this single ECG.
Continuing My System — Regarding R Wave Progression:
The zone of "Transition" — is said to occur where the height of the R wave becomes taller than the depth of the S wave in the chest leads. Transition is normally seen between lead V2-to-V4. Because of common usage — I've retained the term, "R wave progression" as part of my Systematic Approach to 12-lead interpretation — though defining the zone of "transition" provides us with more useful information (See ECG Blog #269 — for full review on R Wave Progression).
- R Wave Progression: In Figure-1 — R wave progression is "poor", because transition is delayed to between lead V4-to V5.
- Other than the QS complex in lead V1 — Q waves and/or QS complexes are not seen in other chest leads. That said — the delayed transition is relevant in today's case! This is because the reduced r wave amplitude in anterior leads, and small size of the R waves in leads V5 and V6 — may reflect loss of anterior forces from recent infarction.
Finally — Regarding ST-T Wave Changes:
ST-T wave abnormalities (some subtle — some not subtle) are seen in at least 9 of the 12 leads in today's tracing. For clarity — I've labeled some of these findings in Figure-2:
- The most remarkable abnormal ST-T wave findings — are the hyperacute T waves in leads V2-thru-V6. It is challenging to define the term, "hyperacute" in reference to T wave appearance. My definition is that in the "right" clinical setting (ie, in a patient with cardiac-sounding chest pain) — 1 or more T waves take on a "hypervoluminous" appearance — in that they appear taller-than-expected given QRS amplitude in the lead being looked at — as well as being "fatter"-at-their-peak and wider-at-their-base than would normally be expected (See ECG Blog #218, as well as the Audio Pearl in that post for more on defining hyperacute T waves).
- The 3 leads in Figure-2 in which T waves are most obviously "hyperacute" — are leads V3, V4 and V5. In each of these leads — T waves tower over the small-amplitude R waves. Not only are these T waves much taller than the R waves — but these T waves are clearly "fatter"-at-their-peak and wider-at-their-base than one would expect, given the size of the R waves (and QRS complex) in these respective leads.
PEARL #3: By the concept of "patterns of neighboring leads" — Since the ST-T waves in leads V3, V4 and V5 are so obviously abnormal — the somewhat less obvious ST-T wave changes in neighboring leads V2 and V6 are also most probably abnormal.
- In lead V6 — although the T wave is not taller than the R wave — this T wave in lead V6 is still much taller-than-one-would-expect given small size of the R wave in this lead.
- Height of the T wave in lead V2 is not as pronounced as T wave amplitude in lead V3. However, the ST segment "takeoff" is unusually straight (ie, parallel to the slanted RED line in lead V2 of Figure-2). In addition, considering how small the r wave is in lead V2 (ie, 2 mm) — the T wave in this lead is once again "hypervoluminous" (ie, clearly with a much-wider-than-it-should-be base). I would therefore interpret leads V2 and V6 as also being "hyperacute".
- ST-T wave changes in lead V1 are subtle — but nevertheless "real". Normally in this lead — there is no more than minimal ST elevation. Although the T wave in lead V1 may normally be inverted (PURPLE arrow in Figure-2) — the shape of the ST segment in this lead (ie, coved or "frowny"-configuration, as schematically shown by the curved RED arc) — in association with the ST elevation seen (with respect to the dotted RED line in lead V1 — showing the PR segment baseline) is not a normal finding (especially given obvious ST-T wave abnormalities in the 5 other chest leads)!
 |
| Figure-2: I've labeled some of the abnormal ST-T wave changes from Figure-1. |
Regarding ST-T wave Changes in the Limb Leads:
- The ST-T waves in leads II, III and aVF are all clearly abnormal. ST segments in each of these inferior leads are "scooped", with suggestion of slight ST depression. That said — the most remarkable finding is the terminal T wave positivity in each of these 3 inferior leads (upward-pointing BLUE arrows in Figure-2 — with the most prominent terminally positive T wave being seen in lead II).
- Depending on the clinical situation (and the stage of evolution during an acute cardiac event) — this finding of terminal T wave positivity in association with ST flattening or depression is clearly abnormal, and may represent the beginning reperfusion changes (ie, the mirror-image of inverting T waves in leads which manifested ST elevation).
- Without the benefit of a prior (baseline) ECG for comparison — I was uncertain if the ST-T waves in leads I and aVL were abnormal. I thought the apearance of the QRST complex in lead aVR was unremarkable.
PEARL #4: When assessing an ECG for the possibility of acute ischemic heart disease — the more leads that are abnormal, the greater the chance that the abnormalities you identify are real! I find it helpful to start with a few leads that obviously show acutely abnormal ST-T wave findings — and then to apply the concept of "patterns of neighboring leads" as I look closely to identify more subtle findings in the remaining leads.
- As described above in Figure-2 — We have identified definite ST-T wave abnormalities in no less than 9/12 leads. This provides strong support in favor of a recent (or still ongoing) cardiac event.
Putting It All Together:
The ECG in Figure-2 shows sinus rhythm — low voltage — a question about a QS in lead III (with a tiny, fragmented complex in lead aVF) — poor R wave progression (with low-amplitude R waves until leads V5, V6) — worrisome hyperacute T waves in leads V2-thru-V6 — with apparent reciprocal ST-T wave changes in the inferior leads (including terminal T wave positivity that probably represents upright reperfusion T waves).
- Given the history of 3 days of symptoms in this older man who finally presented to the ED because of worsening chest pain — I interpreted this tracing as suggesting acute and/or ongoing extensive anterior infarction. Although none of the chest leads manifest J-point ST depression — the disproportionately large chest lead T waves are consistent with a deWinter-like T wave pattern (See ECG Blog #183 for "My Take" on this concept). That said — I wasn't certain about WHEN it was during the patient's 3 days of symptoms that acute infarction took place — or whether perhaps there was an ongoing "stuttering" course with spontaneous opening and closure.
- The course of acute infarction is not always "all or none". By this I mean — that the "culprit artery" (most likely the proximal or mid-LAD in today's case) — may acutely occlude — then spontaneously reopen — followed by spontaneous reopening and reclosure a number of times until a final state is reached for the "culprit" artery.
- Regardless of when during the patient's 3 days of symptoms acute coronary occlusion first occurred — the lack of anterior Q waves, in association wth marked hyperacute T wave changes in this patient who presented to the ED for increased symptoms — strongly suggests that there is still a large area of jeopardized myocardium that may benefit from prompt reperfusion. Cardiac cath was clearly indicated to define the anatomy and guide clinical decision-making.
Case CONCLUSION:
Cardiac cath was performed on the patient in today's case. Not surprisingly, this revealed total occlusion of the mid-LAD (Left Anterior Descending) coronary artery. Minor lesions were found in the LCx (Left Circumflex) and RCA (Right Coronary Artery).
- This patient subsequently developed arrhythmias — that I discuss as this case is continued in my next ECG Blog #273.
==================================
Acknowledgment: My appreciation to 유영준 (from Seoul, Korea) for making me aware of this case and allowing me to use this tracing.
==================================
Related ECG Blog Posts to Today’s Case:
- ECG Blog #205 — Reviews my Systematic Approach to 12-lead ECG Interpretation (outlined in Figures-2 and -3, and the subject of Audio Pearl MP-23-LINK in Blog #205).
- ECG Blog #269 — Reviews assessment of R-Wave Progression (with a Video Pearl in this post on the subject).
- ECG Blog #218 — Reviews of the concept of WHAT is a "Hyperacute" T Wave (Also see the Audio Pearl in this post).
- ECG Blog #183 — Reviews a case of deWinter-like T Waves (with the Audio Pearl in this post discussing some variants of the deWinter T wave pattern).
- ECG Blog #53 — Reviews another case of deWinter T Waves.
- ECG Blog #258 — Reviews the concept of HOW to "Date" an Infarction (Also see the Audio Pearl in this post).
- ECG Blog #193 — illustrates use of the Mirror Test to facilitate recognition of acute Posterior MI. This blog post reviews the basics for predicting the "culprit artery". NOTE: The Audio Pearl reviews the concept of why the term "OMI" ( = Occlusion-based MI) should replace the more familiar term STEMI.
- ECG Blog #262 — Reviews a case of recent acute Infero-Postero MI with group beating from Wenckebach conduction and Low Voltage (with a list of the causes of Low Voltage).
- The January 24, 2020 post in Dr. Smith's ECG Blog — Reviews a case in which Low Voltage (with progressive reduction in QRS amplitude on serial ECGs) was due to myocardial stunning (See My Comment at the bottom of the page).
- The November 12, 2020 post in Dr. Smith's ECG Blog — Reviews a case in which Low Voltage was seen in a patient with Covid-19 and cardiogenic shock, in which low voltage seemed to precede (? predict) reduced LV function! (See My Comment at the bottom of the page).